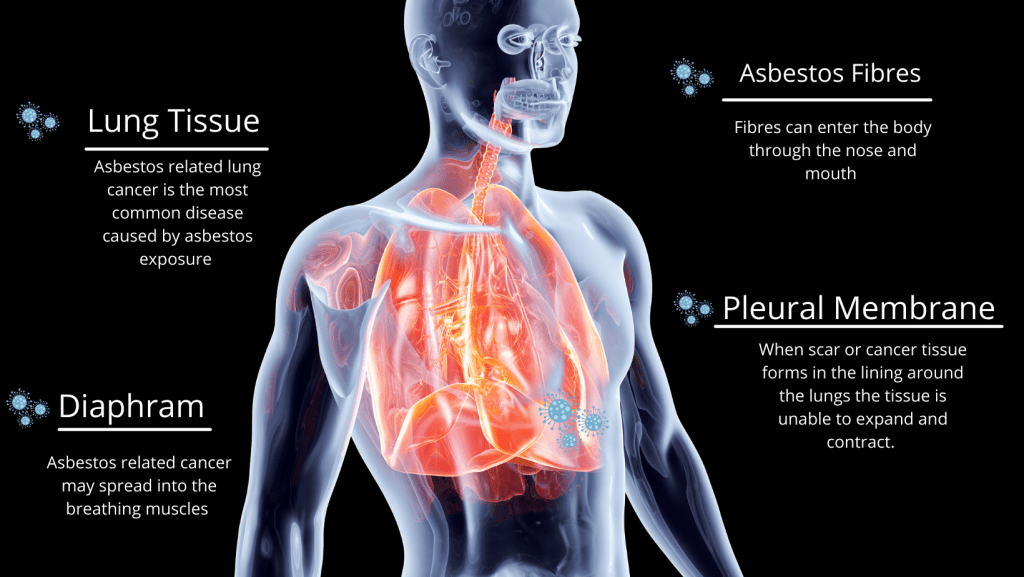
When professionals in construction, building management or occupational safety hear the word asbestos, they may think of old insulation, legacy building materials or regulatory checklists. Yet the real story, how asbestos exposure affects health, remains critically important and still evolving. In this article you’ll learn what asbestos exposure means for workers and public health, understand the diseases it causes, review key statistics, and explore how to translate that knowledge into practical workplace action.
What is Asbestos?
Definition and uses
Asbestos is a group of naturally occurring fibrous minerals known for heat- and corrosion-resistance. Historically, it was used in insulation, floor tiles, cement products, brakes and numerous building materials.
Exposure pathways
The primary health risk arises when asbestos-containing materials are damaged or disturbed, releasing microscopic fibers into air. People inhale or, less commonly, ingest these fibers. Ambient exposure (living near asbestos sources) or occupational exposure (working with asbestos) are both concerns.
Latency and cumulative risk
One hallmark of asbestos‐related health impact is latency, diseases often appear decades after exposure. Also, risk correlates with amount, duration and fibre type/characteristics of exposure.
Health Effects of Asbestos Exposure
Non-malignant lung and pleural diseases
- Asbestosis – Progressive scarring of lung tissue from inhaled asbestos fibres; signs include shortness of breath, dry cough, chest tightness.
- Pleural plaques, pleural thickening and pleural effusions – Changes to the lung linings (pleura) without necessarily becoming cancer, but markers of exposure.
- These conditions reduce lung flexibility and function, creating vulnerability in affected workers.
Cancers associated with asbestos
All major health authorities agree: asbestos is a human carcinogen.Key cancers:
- Mesothelioma – Rare but aggressive cancer of the lining of lungs/abdomen; strongly linked to asbestos.
- Lung cancer – Exposure to asbestos significantly increases lung cancer risk.
- Cancers of the larynx, ovary and possibly stomach, colorectum and pharynx have also been linked.
Magnitude of the burden – statistics
- Globally, millions of workers were exposed historically; the World Health Organization estimates that “all six main forms of asbestos have been assessed by WHO as carcinogenic to humans.”
- A 2017 review estimated ~255,000 deaths per year worldwide attributable to asbestos. (
- In the U.S., mortality from occupational asbestos exposure increased by ~20% from 1990 to 2019, even though age-standardised rates declined.
- In a cohort with asbestosis (Chinese hospital-based), Standardised Incidence Ratios (SIRs) were: lung cancer SIR ~16.6, mesothelioma ~175.
- In Sweden construction workers were heavily exposed, relative risk (RR) of lung cancer was ~1.74 (CI 1.25-2.41) compared to low exposure.
Interaction with other risk factors
- Smoking and asbestos exposure together produce much higher lung cancer risk than either alone.
- Environmental (non-occupational) exposure still carries measurable risk: for example, in Britain the lifetime mesothelioma risk from environmental asbestos exposure among people born since 1965 is ~1 in 10,000.
Why Asbestos Still Matters for Professionals
Legacy buildings and hidden hazards
Though many uses of asbestos are banned or restricted in some countries, asbestos-containing materials remain in older buildings, industrial sites, shipyards, etc. Disturbing or modifying these materials (e.g., during renovation or demolition) can release fibers. As professionals you must remain vigilant.
Long latency means current exposures translate to future disease
Because diseases may take 20-40 years to manifest, actions taken now matter for decades.
Regulatory & legal implications
Many jurisdictions require risk assessment, safe removal (abatement), monitoring and worker protection when asbestos is present. Failure to manage asbestos appropriately can expose organisations to liability and health risk.
Practical Steps for Risk Management
Identifying asbestos risks
- Conduct thorough surveys for asbestos-containing materials (ACMs) especially in older buildings
- Prioritise friable materials (those easily crumbled/released) for safe handling or removal.
- Document exposure history for workers and contractors (duration, material type, tasks performed).
Controlling exposure
- When ACMs must be disturbed: use appropriate containment, ventilation, HEPA filtration, and personal protective equipment (PPE with respirators)
- Avoid DIY or uncontrolled removal by untrained staff – best left to certified abatement professionals.
Monitoring & health surveillance
- For workers with potential exposure: establish medical surveillance, lung function testing/imaging where appropriate
- Encourage smoking cessation – since smoking + asbestos exposure dramatically escalates risk.
- Maintain records of exposures, even if workers move roles or retire, because of latency.
Policy and prevention culture
- Develop organisational policy that treats asbestos as a persistent hazard, not merely a legacy issue
- Educate teams (maintenance, facilities, construction) on recognising, reporting and safely managing asbestos
- Engage external expertise for removal, abatement or safe management of existing materials.
Tailoring Advice for Professional Audiences
For Occupational Health & Safety (OHS) practitioners
Frame asbestos as a chronic risk – the hazard may not manifest immediately but consequences are severe and delayed. Use data-driven risk assessments and integrate asbestos hazard into workplace safety management systems.
For Building/Facilities Managers
You are custodians of infrastructure risk. Treat asbestos-containing assets like any other ageing hazard: ensure inventories, condition assessments and maintenance/refurbishment plans incorporate asbestos risk.
For Consultants & Legal Advisors
Given the legal and regulatory implications, ensure documentation of material surveys, exposure histories, training records, and abatement work. The statistical evidence of disease burden strengthens the case for rigorous management.
Conclusion
Understanding how asbestos affects health is more than academic—it’s a real, measurable risk with consequences spanning decades. We’ve covered what asbestos is, how exposure happens, the diseases it causes, and why professionals in construction, facilities management, occupational health and compliance must stay alert. The statistics make it clear: thousands die each year from asbestos-related diseases; many more workers remain exposed. The upside? With rigorous management and safe practices, the worst outcomes are preventable. Are you confident your organisation’s asbestos-risk programme is equipped for today’s reality and tomorrow’s legacy?
FAQs
Q1: How soon after exposure to asbestos will disease show up?
Diseases such as lung cancer or mesothelioma often appear 20-40 years after first exposure.
Q2: Is there a “safe” level of asbestos exposure?
No internationally recognised “safe” level exists—any exposure carries some risk, especially long-term or high-concentration exposures.
Q3: Does asbestos only affect workers who directly handle it?
No. Occupational exposure is the highest risk, but environmental exposure (e.g., living near asbestos sources, second-hand exposure via workers) also carries measurable risk.
Q4: If a worker is exposed, what actions should be taken?
Document the exposure, ensure ongoing hazard control, provide medical monitoring, encourage smoking cessation, and if removal from exposure is possible, plan accordingly.
Q5: Are certain materials safer than others regarding asbestos?
Materials where asbestos fibres are well-bonded and undisturbed pose lower immediate risk, but if damaged, disturbed or degraded, fibres can be released. Always assume potential hazards and manage accordingly.